User:Mychm52/sandbox
From Wikipedia, the free encyclopedia
Bonnet-Dechaume-Blanc syndrome, also known as Wyburn-Mason Syndrome, is a rare congential arteriovenous malformation of the brain, retina or facial nevi.[1] The syndrome has a number of possible symptoms and can affect the skin, bones, kidneys, muscles, and gastrointestinal tract.[2] When the syndrome affects the brain, people can experience severe headaches, seizures, acute stroke, meningism and progressive neurological deficits due to acute or chronic ischaemia caused by arteriovenous shunting.[2][3]
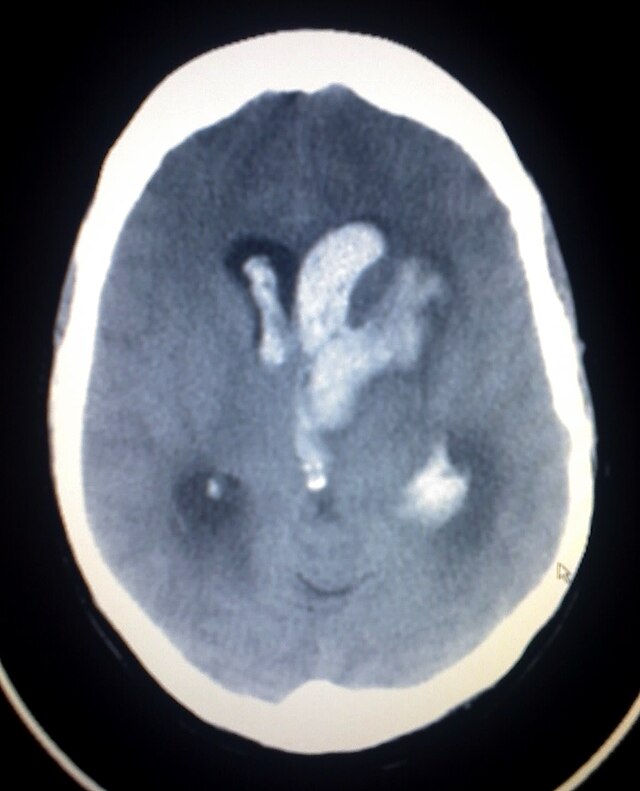
As for the retina, the syndrome causes retinocephalic vascular malformations that tend to be present with intracranial hemorrhage and lead to decreased visual acuity, proptosis, pupillary defects, optic atrophy, congestion of bulbar conjunctiva, and visual field defects.[4][5] Retinal lesions can be unilateral and tortuous, and symptoms begin to appear in the second and third decades of life.[3][5]
The syndrome can present cutaneous (pertaining to the skin) lesions, or skin with different texture, thickness, and color, usually on the face.[4] The facial features caused by the syndrome vary from slight discoloration to extensive nevi and angiomas of the skin.[5] In some cases, the frontal and maxillary sinus can present problems in the subject due to the syndrome.[4]
There have only been 52 reported cases of patients with Bonnet-Dechaume-Blanc syndrome as of 2012.[2] Bonnet-Dechaume-Blanc syndrome is caused by a congenital disorder that is developed by disruption of developing tissues that lead to abnormalities in vascular tissues of the eye.[4] Symptoms are rarely noticed in children and the syndrome is often diagnosed in late childhood or early adulthood when visual impairment is noticed.[3] Fluorescein angiography is commonly used to diagnose the syndrome.[6]
There have been controversies on treatment for patients who display Bonnet-Dechaume Blanc syndrome. Patients with intracranial lesions have been treated with surgical intervention and in some cases, this procedure has been successful. Other treatments include embolization, radiation therapy, and continued observation.[4]
Since the syndrome is rare and non-heritable, research has been focused on the clinical and radiological findings rather than how to manage the syndrome.[3]