
Clostridioides difficile
Species of bacteria / From Wikipedia, the free encyclopedia
Dear Wikiwand AI, let's keep it short by simply answering these key questions:
Can you list the top facts and stats about Clostridioides difficile?
Summarize this article for a 10 year old
Clostridioides difficile (syn. Clostridium difficile) is a bacterium known for causing serious diarrheal infections, and may also cause colon cancer.[4][5] It is known also as C. difficile, or C. diff (/siː dɪf/), and is a Gram-positive species of spore-forming bacteria.[6] Clostridioides spp. are anaerobic, motile bacteria, ubiquitous in nature and especially prevalent in soil. Its vegetative cells are rod-shaped, pleomorphic, and occur in pairs or short chains. Under the microscope, they appear as long, irregular (often drumstick- or spindle-shaped) cells with a bulge at their terminal ends (forms subterminal spores). Under Gram staining, C. difficile cells are Gram-positive and show optimum growth on blood agar at human body temperatures in the absence of oxygen. C. difficile is catalase- and superoxide dismutase-negative, and produces up to three types of toxins: enterotoxin A, cytotoxin B and Clostridioides difficile transferase.[7] Under stress conditions, the bacteria produce spores that are able to tolerate extreme conditions that the active bacteria cannot tolerate.[8]
| Clostridioides difficile | |
|---|---|
 | |
| C. difficile colonies on a blood agar plate | |
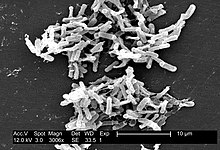 | |
| Electron micrograph of the bacterium | |
| Scientific classification | |
| Domain: | Bacteria |
| Phylum: | Bacillota |
| Class: | Clostridia |
| Order: | Eubacteriales |
| Family: | Peptostreptococcaceae |
| Genus: | Clostridioides |
| Species: | C. difficile |
| Binomial name | |
| Clostridioides difficile (Hall & O'Toole, 1935) Lawson & Rainey, 2016 | |
| Synonyms | |
Clostridioides difficile is an important emerging human pathogen; according to the CDC, in 2017 there were 223,900 cases in hospitalized patients and 12,800 deaths in the United States.[9] Although C. difficile is commonly known as a hospital and antibiotic associated pathogen, at most one third of infections can be traced to transmission from an infected person in hospitals,[10] and only a small number of antibiotics are directly associated with an elevated risk of developing a C. difficile infection (CDI), namely vancomycin, clindamycin, fluoroquinolones and cephalosporins.[11][12][13] The majority of infections are acquired outside of hospitals, and most antibiotics have similar elevated risk of infection on par with many non-antibiotic risk factors, such as using stool softeners and receiving an enema.[14]
Clostridioides difficile can also become established in the human colon without causing disease.[15] Although early estimates indicated that C. difficile was present in 2–5% of the adult population,[8] more recent research indicates colonization is closely associated with a history of unrelated diarrheal illnesses, such as food poisoning or laxative abuse.[16] Individuals with no history of gastrointestinal disturbances appear unlikely to become asymptomatic carriers. These carriers are thought to be a major reservoir of infection.[17]